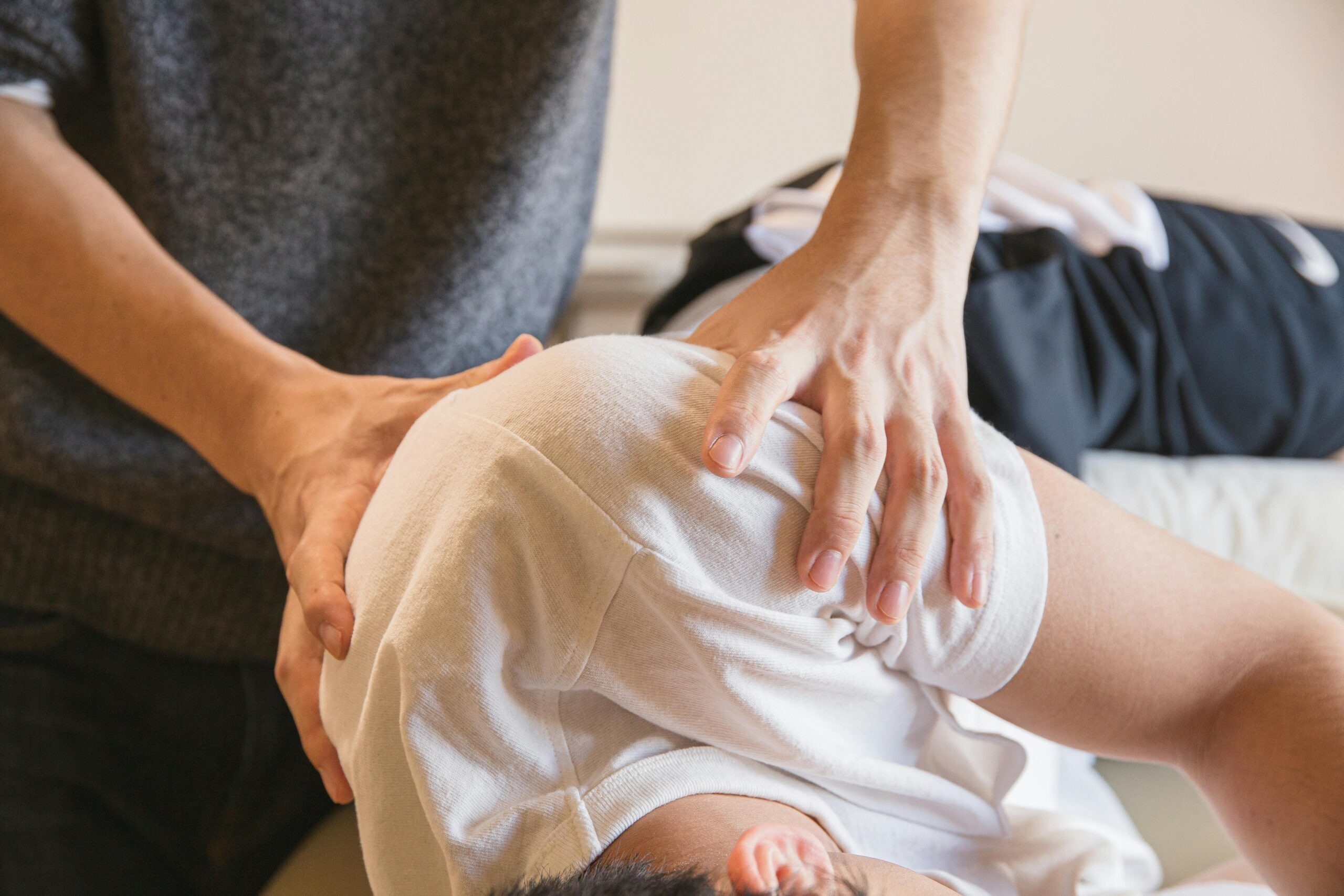
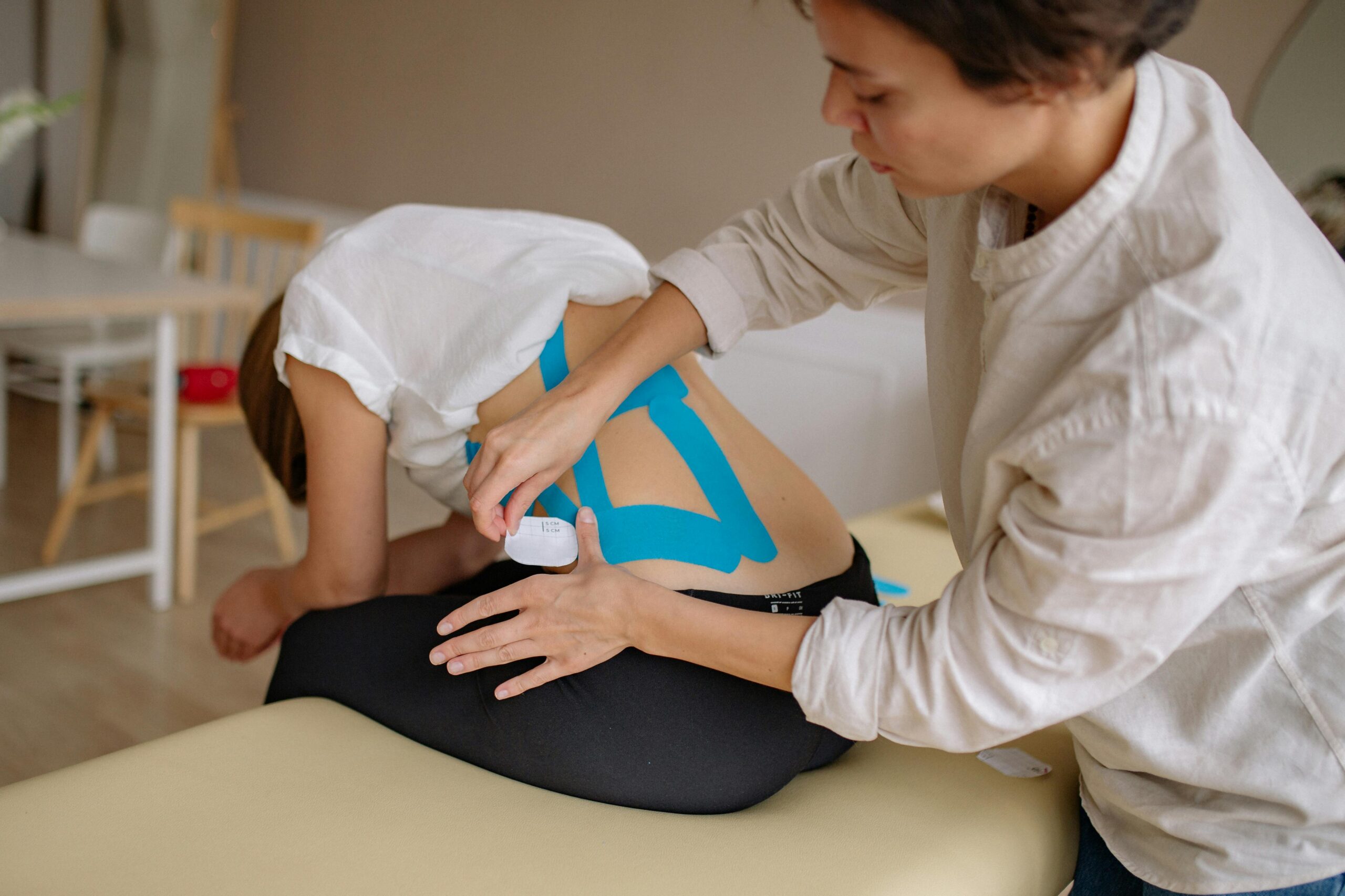
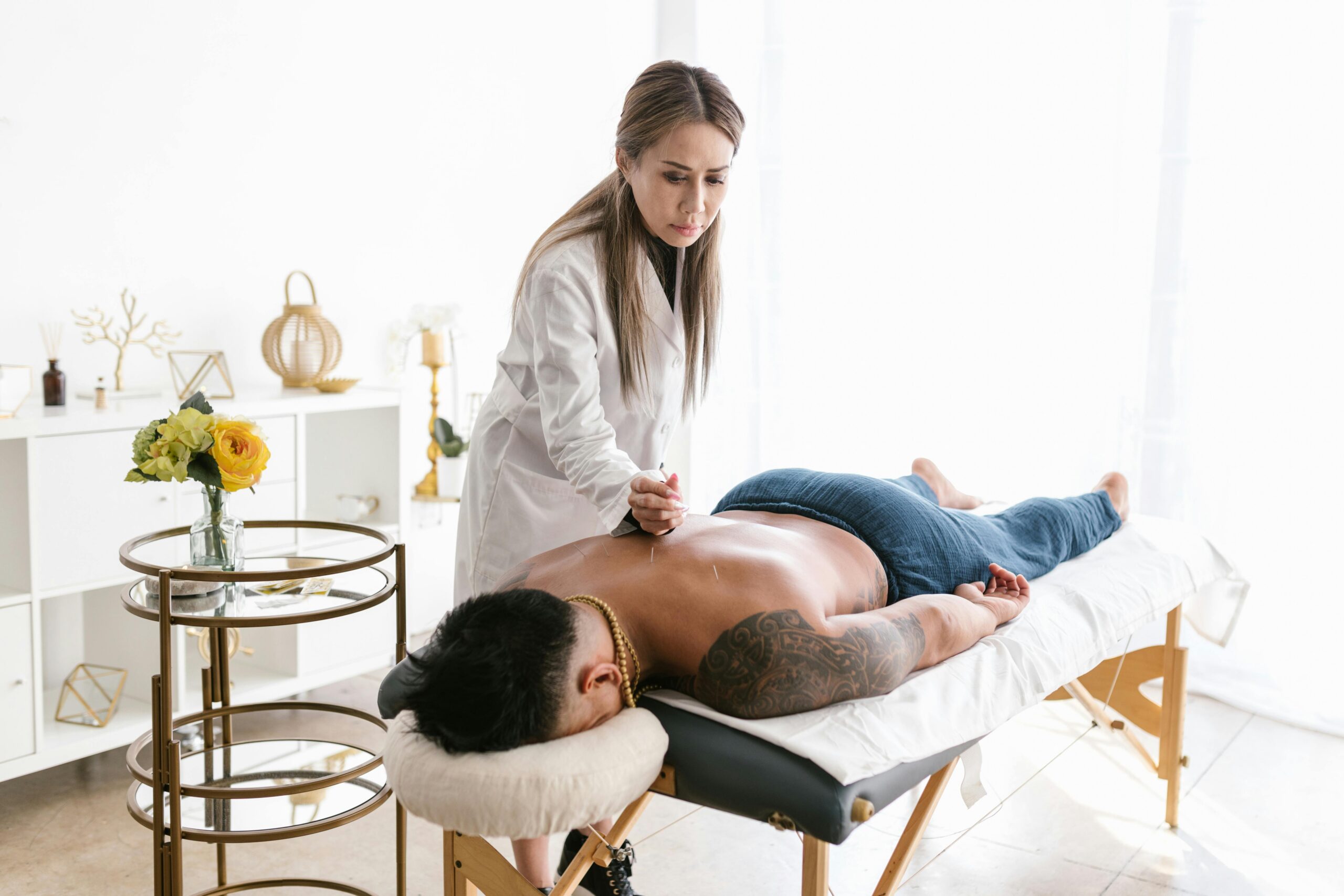
Physiotherapy for back pain is the cornerstone
The best treatment for most back pain is physiotherapy that combines assessment, targeted exercise, and load management.
Not passive treatment on its own.
Not generic “core” work.
Not a scan and a shrug.
Good physiotherapy earns its value in three ways.
1. It identifies the driver, not just the location
A sore middle back might be thoracic stiffness plus poor rib mobility, not “tight muscles.”
Lower back pain might be a hip-dominant lifting strategy that overloads lumbar tissues when fatigue sets in.
Example: the gym-goer who deadlifts fine early in the session, but after accessories their form shifts, their brace disappears, and the lumbar spine takes the hit. The fix is not “avoid deadlifts forever.” It’s capacity, technique under fatigue, and graded exposure.
1. It gives you a progression that matches your life
One-size programs fail because people don’t live one-size lives.
A nurse doing 12-hour shifts needs a plan that accounts for:
- – repeated bending at awkward angles,
- – time pressure,
- – sleep disruption.
A tradie needs:
- – lifting tolerance,
- – rotation control,
- – realistic strategies for “I can’t take two weeks off.”
3. It reduces fear and restores confidence
Fear changes movement.
People with back pain often brace, avoid bending, and move in slow rigid blocks. That pattern amplifies load in the wrong places and keeps the system irritable.
A good physio doesn’t just “fix tissue.” They help you move normally again, and that’s often the difference between recovery and recurrence.
Exercise: what works depends on the pattern, not the trend
Let’s get specific.
Scenario A: acute lower back pain after lifting (no leg symptoms)
Early goals: reduce sensitivity, keep function.
A starting point might be:
- – 5–10 minute walks, 3–5 times/day
- – hip hinge drill with dowel to reintroduce bending
- – isometric holds: e.g., side plank (short lever) 3 x 10–20 seconds
- – glute bridges 2–3 sets, controlled tempo
Then progress toward:
- – goblet squat patterning
- – Romanian deadlift pattern (light)
- – loaded carries (farmer carries) for spinal endurance
Scenario B: sore middle back from desk work
If your upper back feels like it’s “stuck” by 3pm, stretching your neck is rarely the main fix.
You’re usually dealing with:
- – reduced thoracic extension,
- – rib cage stiffness,
- – scapular endurance deficits.
A practical progression:
- – thoracic extension over a foam roller (targeted, 1–2 minutes)
- – wall slides or serratus-focused reaches
- – rowing variations, higher rep endurance
- – “movement snacks” across the day: 60 seconds every hour beats 10 minutes once
Scenario C: recurring back pain with sitting and driving
If sitting flares you, the answer isn’t “sit perfectly.”
It’s:
- – vary positions (seat tilt, lumbar support adjustment),
- – standing breaks,
- – build tolerance with gradual exposure.
We’ve seen people transform their symptoms by doing one boring thing consistently: standing up every 30 minutes and walking for two minutes. It’s not glamorous. It works.