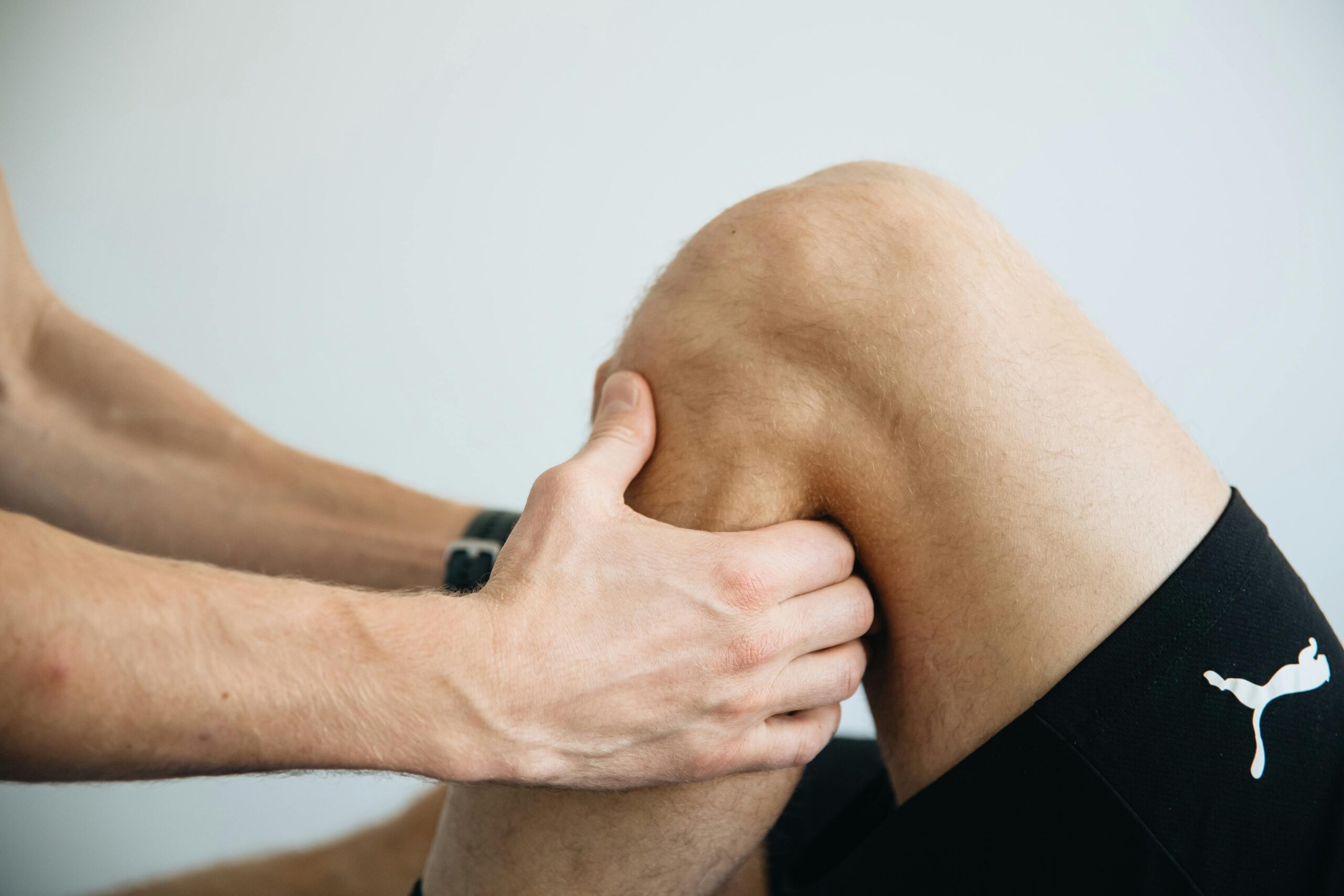
“Can a torn ACL heal without surgery?” is often asked as if the answer should be yes or no, like asking whether a broken finger needs a splint. But ACL injuries do not behave that neatly.
Yes, some torn ACLs show signs of healing without reconstruction.
No, that does not mean most active people can safely ignore instability, do a few band exercises, and get back to cutting and pivoting in sport.
What an ACL Tear Really Changes
The ACL is not just “a ligament in the knee.” It is a primary restraint against anterior translation of the tibia and a major contributor to rotational control. In plain terms, it helps stop the knee from shifting and twisting into positions it cannot tolerate under speed.
That is why ACL tears are common in sport situations that combine deceleration, change of direction, and poor force absorption. Think of a netball player landing slightly off-centre after contesting a pass. Or a footballer planting to cut inside while the trunk drifts laterally and the knee falls into valgus. Or a skier catching an edge with the body still moving downhill.
These are not random accidents. They are specific mechanical problems occurring at high speed.
Once the ACL tears, the issue is not just pain. Pain usually settles. Swelling usually settles. The harder question is whether the knee remains trustworthy when speed, fatigue, and unpredictability return.
Can It Heal Without Surgery? Yes. But That Is Not the Whole Question
Some clinicians cite MRI evidence of ACL healing and jump straight to a hopeful conclusion. However, tissue continuity on imaging is not the same thing as a knee that tolerates late-stage acceleration, contact, reactive cutting, or rotational load.
A better way to frame it is this: an ACL may demonstrate biological healing, partial continuity, or functional compensation without surgery. The real issue is whether that outcome is enough for the demands placed on the knee.
A 42-year-old parent who wants to lift weights, hike, coach junior sport, and jog twice a week is solving a different problem from a 19-year-old winger who needs to decelerate off the right leg, cut left, and explode into open space fifteen times a match.
Lumping those people into the same answer should not be the case.