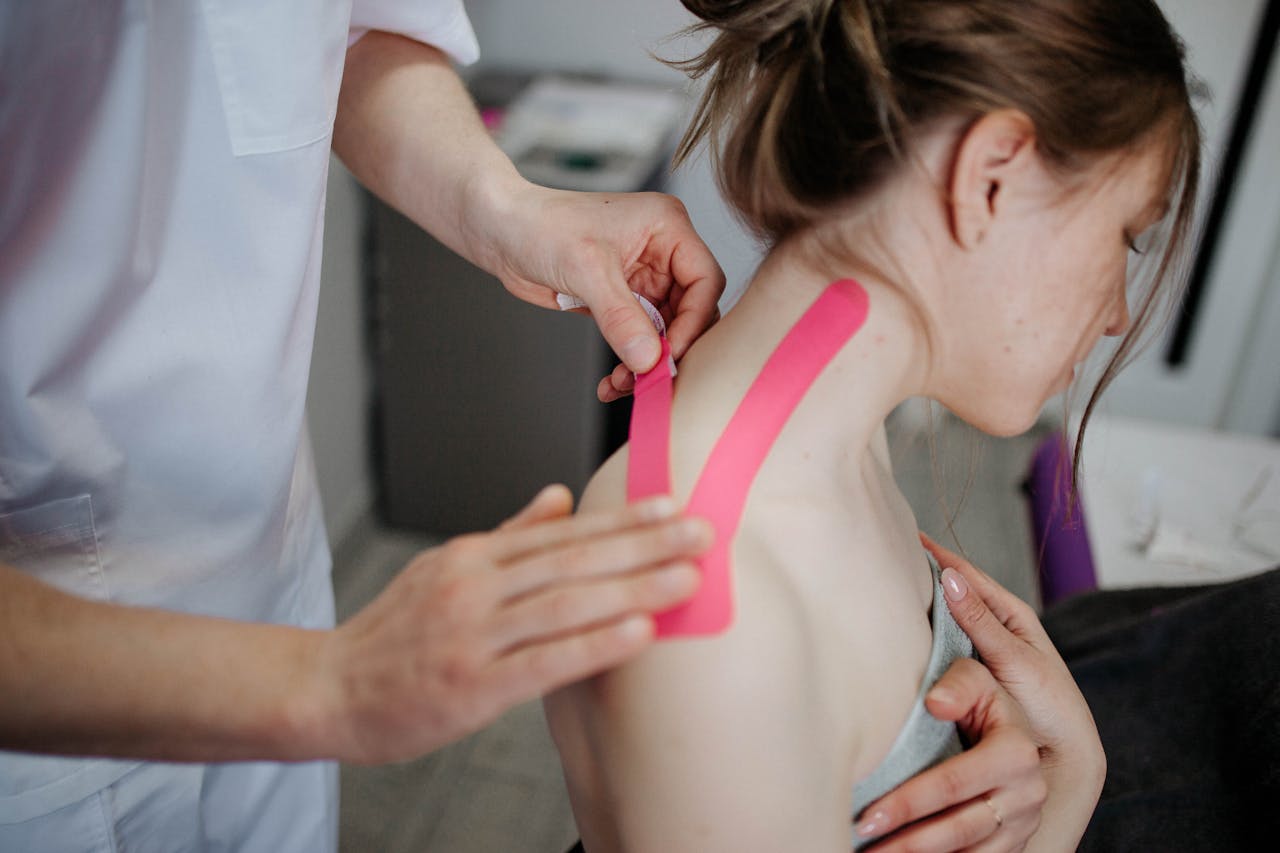
The 3 Stages of Frozen Shoulder (And What Each One Feels Like)
The staging model is what dictates treatment.
Freezing Stage
Pain is dominant. Often most severe at night. Patients struggle to lie on the affected side. Attempting aggressive stretching here is a mistake. It amplifies irritability.
Frozen Stage
Pain may reduce slightly, but stiffness becomes more pronounced. A patient might report, “It doesn’t hurt as much, but I can’t move it.” This is where functional limitations peak.
Thawing Stage
Gradual return of movement. Progress is slow but measurable. This is where more assertive mobility work becomes appropriate.
Treating all stages with the same protocol is poor practice. Yet it happens frequently.
Physio Treatment for Frozen Shoulder: What Actually Helps
Let’s be clear. There is no single “fix.”
Effective physio treatment is stage-specific and load-sensitive.
Hands-On Physiotherapy Techniques
Joint mobilisation can be useful, particularly in the frozen and thawing stages.
But the idea that manual therapy alone will “break adhesions” is outdated. What it can do is improve tolerance to movement and provide short-term gains in range.
Those gains must be reinforced with active movement. Otherwise, they are transient.
Exercise-Based Rehab (The Most Important Part)
This is where outcomes are determined.
In the freezing stage, the goal is not to restore full range. It is to maintain available movement without increasing irritability. Pendulum exercises and supported range work are often appropriate.
In the frozen stage, more structured mobility work is introduced. For example, assisted active external rotation with a stick or towel, performed within tolerable limits.
In the thawing stage, loading becomes more important. Strengthening the rotator cuff and scapular stabilisers helps normalise movement patterns.
We’ve seen patients who were told to “stretch aggressively” early on and ended up plateauing for months. In contrast, those who followed a graded, stage-appropriate program progressed more steadily.
That’s not coincidence.
Pain Management Strategies
Pain needs to be managed, not ignored.
Heat before movement can reduce stiffness. Adjusting sleep position, often by supporting the arm in slight abduction, can reduce night pain.
Activity modification is also critical. Completely avoiding movement is not helpful. But repeatedly provoking pain is equally counterproductive.
There is a middle ground, and good physio guidance helps patients find it.
What NOT to Do
This deserves emphasis.
Forcing range in the early stage is one of the most common errors I see. It increases inflammation and prolongs the freezing phase.
Another is over-reliance on passive treatments without active follow-up.
And finally, ignoring progressive stiffness because “it will loosen up.” It often doesn’t, not without appropriate intervention.